Health and Lifestyle
Special Report: Who is eligible for a COVID-19 booster and why should get one now
California and Colorado now recommend boosters for all as urgency grows to boost COVID immunity.
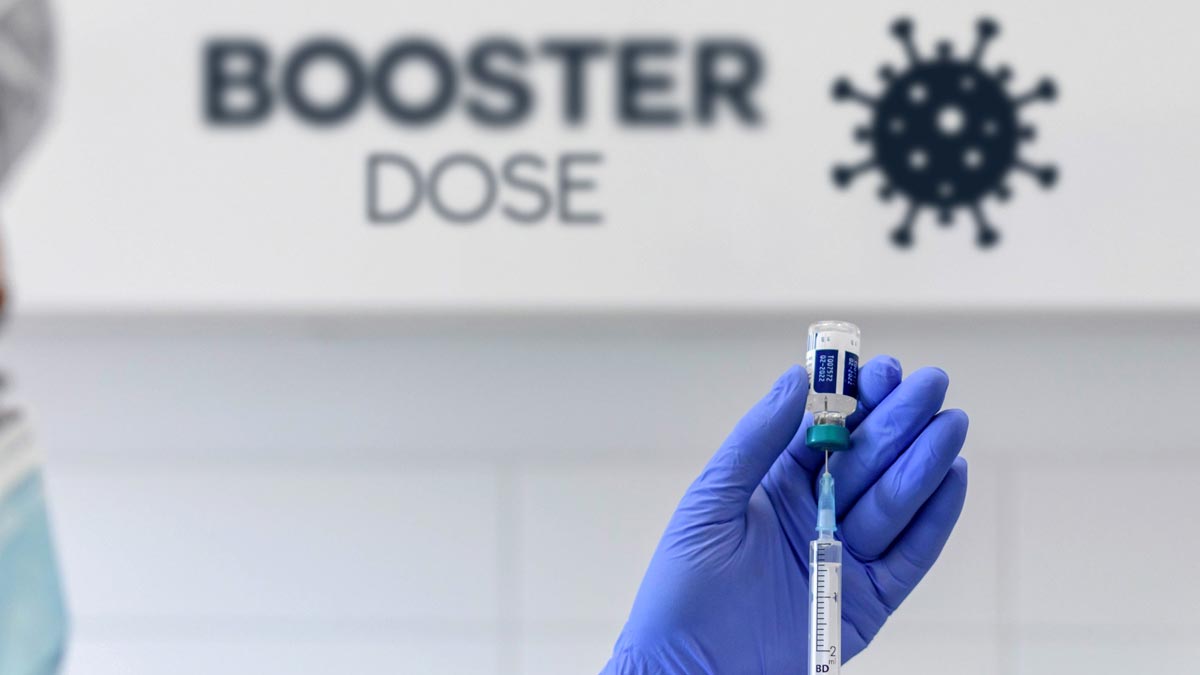
[SEATTLE, Wash.] – (MTN) During a Facebook Live with Congresswoman Anna Eshoo (CA-D) on Tuesday, Dr. Anthony Fauci M.D., Director of the National Institute of Allergy and Infectious Diseases, recommended Americans who are eligible to get a Covid-19 booster shot to get one as soon as possible due to waning immunity.
With concern growing about a sixth wave in states that finished beating back the Delta surge and states such as Colorado, Michigan, Minnesota, and Vermont having a late fifth wave, questions about eligibility for boosters are growing.
Some states aren’t waiting for direction from the federal government. California Governor Gavin Newsom and California Health Secretary Dr. Mark Ghaly told state residents 18 and older they should “absolutely” sign up to get a COVID booster. On Thursday, Colorado Governor Jared Polis issued a directive that defies current federal guidance on Covid-19 booster shots, permitting all state residents 18 and older to get them.
During a White House briefing on Wednesday, Dr. Rochelle Walensky, director of the U.S. Centers for Disease Control and Prevention (CDC), said there continued to be a need to prioritize those who are currently eligible for a Covid-19 booster but added, “as you likely know, FDA is currently looking at the data for expanding boosters to all populations.”
Who is currently eligible for a Covid-19 booster
Eligibility depends on which vaccine you received and several other factors.
Janssen/Johnson & Johnson
If your initial vaccine was Janssen/Johnson & Johnson and you’re 18 or older, you are eligible for a booster 60 days after receiving your first dose. There are no limitations for age, comorbidities, living arrangements, or vocation.
The FDA has approved a mix-and-match approach, and you can receive a booster using the Pfizer or Moderna vaccine or a second Johnson & Johnson dose.
The Johnson & Johnson vaccine has a 1:500,000 chance of causing a rare condition called VITT. In the United States, there have been 47 reported cases and four deaths. If you were assigned female at birth and have a family history of blood clots or low platelets, or you are of childbearing age and using a hormone-based form of birth control, and you’re concerned about VITT, talk to your healthcare provider, OB/GYN, or fertility specialist.
If you’ve had a confirmed case of Covid-19 in the last 90 days and you were symptomatic, talk to your doctor or healthcare provider on whether you should wait to receive a booster.
BioNTech/Pfizer and Moderna
Anyone 65 or older and received the Pfizer or Moderna vaccine is eligible for a booster 180 days after their second dose. People 18 to 64 can qualify for a third dose if they have certain medical conditions, work in a high-risk environment, or live in an area where social distancing isn’t feasible.
Medical conditions that put you at risk for severe Covid-19
If you are 18 to 64 and have any of these conditions, you qualify for a booster.
- Cancer or a prior history of cancer
- Chronic kidney disease
- Chronic liver disease
- Chronic lung disease such as moderate to severe asthma, bronchiectasis, COPD including obstructive sleep apnea, fibrosis or prior lung damage due to scarring, injury, or prior disease, cystic fibrosis, pulmonary embolism or history of, or pulmonary hypertension or history of
- Dementia or Alzheimer’s
- Diabetes – Type 1 or Type 2
- Down Syndrome
- Heart disease such as heart failure, coronary artery disease, high blood pressure, cardiomyopathies
- HIV
- Immunocompromised, auto-immune disease, taking immunosuppressants, or using drugs that suppress the immune system such as steroids both oral and topical
- Mental health conditions including mood disorders, depression, and schizophrenia
- Body Mass Index (BMI) over 25
- Pregnant, trying to get pregnant, or sexually active and could get pregnant and would carry pregnancy to term
- Sickle cell disease or Thalassemia
- Smoking or vaping currently or in the past
- Solid-organ or blood stem cell transplant
- Stroke or cerebrovascular disease
- Substance abuse past or present including alcohol, opiods, or cocaine
- Tuberculosis
Living conditions
If you have any of these living arrangements, you qualify for a booster.
- Long-term care facility
- Homeless shelter – short or long term
- Jail or prison inmate
- Community living arrangements such as dormatories, halfway houses, group homes, or hostels
- Live with a high-risk individual with a medical condtion listed above, or live in a multi-generational household, and you are the primary care provider
Work exposure
If you work in an environment where you interact with Covid-19 positive people or have significant contact with the public, you are eligible for a booster.
- First responders such as healthcare workers, firefighters, police, or congregate care providers
- Educational staff such as teachers, support staff, athletics staff, transportation, and daycare workers
- Food and agriculture workers
- Manufacturing workers
- Correctional officers and employees who work in jails or prisons including healthcare, educators, and mental health providers
- U.S. Postal Service workers
- Public transit workers
- Grocery store workers and other retail and service employees that have high contact with the public
There have been less than 1,000 mild to moderate myocarditis cases in the United States connected with receiving the mRNA Pfizer or Moderna vaccines. Most of these cases involved adolescents or young men. If you were assigned male at birth and have a history of heart disease, or are worried about myocarditis, talk to your healthcare provider to see if the Jassen/Johnson & Johnson vaccine is a better option.
Just like the J&J vaccine, If you’ve had a confirmed case of Covid-19 in the last 90 days and you were symptomatic, talk to your healthcare provider to determine if you should wait to receive a booster.
I thought the COVID vaccine was forever
The idea that the Covid-19 vaccine would be one and done is a creation of misinformation, misunderstanding, and poor reporting by some news outlets.
As the first COVID wave was winding down in the United States in May 2020, there were discussions about having “immunity passports.” People who had a confirmed Covid-19 case could be permitted to return to work and other activities based on the assumption they possessed natural immunity. Shortly after the discussions started, early evidence began to pile up that natural immunity was short-lived. The journal Nature Medicine shared a report on June 18 showing natural immunity started to fade after three months.
The closest claim that immunity from natural exposure or vaccination would last a lifetime came from former President Donald Trump in October 2020. Still, even then, he never made a complete claim of lifetime protection. On October 11, 2020 during an interview with Maria Bartiromo, Trump discussed his personal battle with Covid-19.
“It looks like I’m immune for, I don’t know, maybe a long time, maybe a short time,” he said. “It could be a lifetime. Nobody really knows, but I’m immune. So the President is in very good shape to fight the battles.”
As Trump was recovering from COVID and considering if he had “long time” immunity, there was more evidence that natural immunity started to fade after three months and a growing number of reinfection cases. For public health officials, an even bigger concern was many people who got reinfected suffered from more severe cases.
In December, when the first Covid-19 vaccines were about to become publicly available in the United States, the medical community was already cautioning the public it was unknown how long immunity would last.
In January 2021, Dr. Kristen Marks M.D., an infectious disease specialist at New York-Presbyterian, said, “We really don’t know whether you’re still immune a year after vaccination. Some of the clinical trials will study adding a booster in a year and comparing whether that’s better or if the immunity is just as good for two years with the two shots. That remains to be determined.”
Data from the United Kingdom and Israel have shown that all immunity wanes. Although cases grew dramatically in both countries, hospitalizations and fatalities did not match the winter 2020 surges. A vast majority of the hospitalized, critically ill, and deaths were among the unvaccinated. In Israel, an aggressive booster program ended their wave where new cases have drifted downward to early July levels.
How long does natural and vaccine based immunity last
Two different studies were released in October 2021, providing insight into how long natural and vaccine immunity last. Neither offer lifetime protection.
On October 1, a study on the durability of immunity against reinfection by SARS-CoV-2 was published in The Lancet. Researchers predicted that natural immunity had a half-life of 142 to 185 days. Half-life means how long does it take for half of the antibodies for a disease to disappear from a person’s blood serum. The study estimated that after 16 months, the average person would no longer have any natural immunity to Covid-19. However, the study also stated that this would vary widely depending on age, overall health, genetics, and risk factors. The half-life could be as short as 45 days or as long as 31 months.
Three days later, the Lancet published a study on vaccine-based immunity titled Effectiveness of mRNA BNT162b2 COVID-19 vaccine up to 6 months in a large integrated health system in the USA. That study indicated that immunity waned from 30% to 50% after five months depending on the mRNA vaccine administered, age, and Covid-19 variants. Simply put, vaccine immunity and natural immunity, when accounting for a range of factors, have similar half-lives.
The viral-vector vaccine from Johnson & Johnson has received less research and has been administered to approximately 15 million Americans. A third study indicated the J&J vaccine was the least effective of the three available options in the United States, particularly with the Delta variant.
Why aren’t the vaccines 100% effective
It is a common misconception that vaccines are 100% effective, especially in industrialized nations. Due to a combination of high vaccination rates for diseases such as measles, mumps, and polio, and enough immunized people to provide community immunity, it is easy to believe that vaccines are perfect and forever.
For example, polio still exists in several countries, and the U.S. Department of Defense and the CDC recommend a poliovirus booster for anyone traveling to those regions. Certain members of Generation X have been advised to get an updated MMR vaccination because data shows that protection from measles doesn’t last a lifetime. Even Ben Shapiro complained on Twitter in 2015 that his 13-month old son was exposed to pertussis and became severely ill.
When it comes to the COVID vaccines, no one in the medical community said any vaccines were 100% effective, and the data has always been publicly available.
In Phase 3 studies, the Pfizer-BioNTech and Moderna vaccines were 95% effective in the first few months after vaccination. Put simply, “If there were 100 people who would have gotten COVID, it prevented 95 of them from getting it, but it didn’t prevent all 100,” says Dr. Marks. “It definitely provides some protection, but it’s not perfect.”
The Johnson & Johnson vaccine reported a 72% efficacy rate in preventing moderate to severe disease from COVID-19 in the U.S. and was 85% effective in preventing severe disease.
The good news is that early data found that those who did contract COVID-19 after receiving the vaccine did not develop a severe form of the disease. “So even if it doesn’t completely prevent illness, the study data shows that it does reduce the severity,” Dr. Marks said. Ten months later, the early projections have largely come true.
In King County, Washington, 22% of all confirmed Covid-19 infections since January 17 have been breakthrough cases. Eleven percent of people hospitalized were vaccinated, and 15% died of Covid-19 related illness. When the total number of vaccinated versus unvaccinated residents is considered, the effectiveness of vaccines, even as the need for boosters is increasing, is evident.
| Population | Confirmed Cases | Hospitalized | Deaths | |
|---|---|---|---|---|
| Fully vaccinated | 1.633M | 20,252 | 433 | 115 |
| Partial or unvaccinated | 319K | 71,857 | 3,373 | 667 |
Unvaccinated King County residents were 12 times more likely to be hospitalized and 13 times more likely to die of Covid-19 from January 17 to November 3.
Additionally, a comparison of King County, Washington, and Dallas County, Texas, provides additional data on vaccination and public health programs’ impact. King County experienced the first superspreader event in February 2020, the first Covid-19 death, and had the first mass casualty situation at a hospital in the United States. A month later, Texas suffered its first Covid-19 death. Over the next 627 days, King County implemented some of the strictest COVID rules in the nation while Dallas County took a more open approach.
On November 1, Dallas County reported its 5,000 COVID-related death while King County reported 2,022. Simply put, 1 in every 530 residents of Dallas County has died of COVID since March 2020 versus 1 in every 1,137 residents in King County since February 2020.
Will we need to get boosters forever
To answer that question, we need to move away from facts and science and step into the arena of opinion. The short answer is, “maybe,” but it depends on the advancement of medical science, improvements in available vaccines, and our own behavior.
In the short term, the data is clear – peak immunity against current Covid-19 variants lasts 142 to 185 whether it is natural or vaccine-based. A regimen of booster shots will likely be needed every 6 to 12 months over the next few years.
Two antiviral drugs are currently being evaluated in the United States. Molnupiravir by Merck is reported to reduce hospitalizations and deaths by 50%, while Pfizer released a study on a medication they are developing that was 88% effective in early testing. Both drugs are oral and would be game-changers in the treatment of Covid-19.
Another way to get off the booster shot treadmill would be to reach 90% to 95% immunity, reducing the number of available hosts for Covid-19 to a level that the disease can’t widely spread in the population – so-called ‘herd immunity.” Given the resistance of 62 million Americans to get vaccinated, and almost half the world doesn’t have access to the COVID vaccine, that seems unlikely.
A third game-changer would be a new variant that emerges and is far more transmissible than the current dominant Delta strains but with significantly less severe symptoms. A version of Covid-19 that is closer to moderate Influenza in symptoms and lethality and is as contagious as measles would quickly infect the population, run out of hosts, and burn itself out while not overwhelming hospitals. This could also lead to “herd immunity.”
The final possibility is the vaccines themselves get better. The original Salk polio vaccine, authorized in 1955, was 50% effective at preventing infections but 90% effective at preventing hospitalizations. It wasn’t until 1962 when the Sabin oral vaccine replaced the Salk vaccine, that infections dropped 90% after a first dose and 99% after four doses.
If the Covid-19 vaccines follow a similar development path as other vaccines, a more effective version will likely be discovered in the future.
Why didn’t the United States approve boosters for all after the Biden Administration announced its intent
Over the summer, the Biden Administration and the World Health Organization (WHO), FDA, and CDC had a very public disagreement on who should get booster shots. President Biden wanted every adult to be eligible for a booster. The WHO objected, pointing out how some nations had no access to COVID vaccines while the United States was throwing out expired doses. The FDA and CDC also pushed back, arguing there wasn’t enough real-world data to support boosters for all.
While the debate raged, experts had a real-world case study unfolding on the other side of the world. Israeli officials started boosters for anyone over 60 on July 13 and three weeks later dropped the age to 40. On September 25, they dropped the age again to 12 and older. The program was highly effective at controlling deaths and hospitalizations, and when Israel is compared to the United Kingdom, the booster program implemented was an evident success.
On September 22, the FDA approved booster shots for recipients of the Pfizer vaccine, and on October 20 added the vaccine by Moderna. Eligibility was limited to people who were 65 or older or were 18 to 64 and worked or lived in places with a high risk of exposure or had a serious underlying medical condition that increased their chances of severe COVID. The FDA recommended a booster six months after receiving the second dose.
Also, on October 20, the FDA authorized boosters for anyone who received the Johnson & Johnson vaccine. As the Delta variant raged in the southeastern United States during the summer of 2021, it became evident the J&J vaccine offered less protection against hospitalization. Additionally, the viral-vector vaccines created by Astra Zeneca and developed in Russia and China were also low-performing. Anyone who received the Johnson & Johnson vaccine was advised to get a booster 60 days after the first dose.
Unfortunately, the ethical and trust concerns that tainted the debate in the United States have resulted in new COVID cases stuck on a high plateau for the last three weeks. New cases are rising in most states, and the pattern of Covid-19 infections looks eerily similar to the United Kingdom. A vast majority of hospitalized COVID patients continue to be unvaccinated.
The world needs to learn to live with Covid-19 and everyone will eventually have a date with the illness. The question is, will you be effectively vaccinated or not when it happens.